Breadcrumb
Professors’ research reveals clues to long-COVID symptoms and treatment
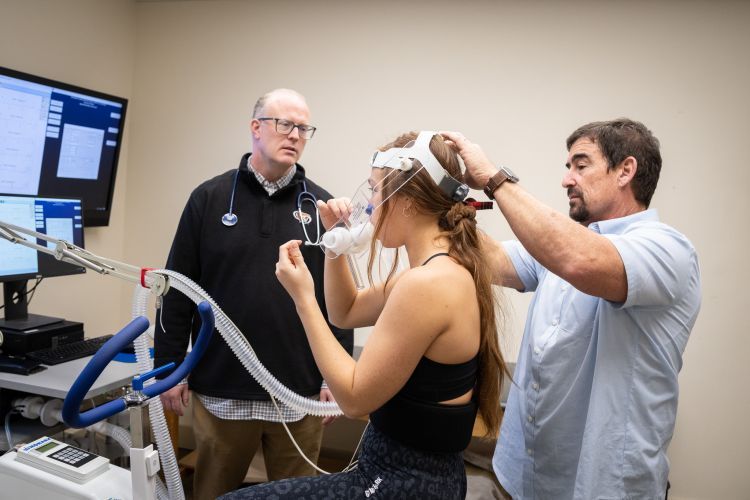
Professor of Physical Therapy Todd Davenport (L) and Professor of Health and Exercise Sciences Mark Van Ness (R)
When Roy Park contracted COVID-19 in December 2020, the symptoms were mild, and he seemed to quickly recover. That changed a few months later.
“I was very active before I got COVID. I worked out six days a week. I was a swimmer. I was a runner. I lifted weights. So it was really shocking and scary to me that I couldn't even go on a five-minute jog,” Park said.
He soon learned the debilitating fatigue—even loading the dishwasher was taxing—is a common symptom of long-COVID. Research from University of the Pacific professors is helping Park and countless others understand what is causing the symptoms and how to manage them.
Long-term effects from COVID-19 can take various forms and last weeks, months or longer. More than 100 million people worldwide are thought to have long-COVID.
Professor of Physical Therapy Todd Davenport and Professor of Health and Exercise Sciences Mark Van Ness have extensively researched and collaborated on post-viral fatigue in other illnesses such as Lyme disease and Epstein-Barr.
“What we had been studying provides insight into what is happening now as long-COVID,” Van Ness said.
Van Ness uses exercise testing to learn the cause of fatigue and other symptoms. “We’re looking at what is broken in the systems that leads to the diverse symptoms people experience,” he said.
While his research has found similarities with other diseases, one significant difference among long-COVID patients is that it can damage lungs. “That’s unique to COVID,” Van Ness said. “We’re not sure if it ever heals. There are some indications that it does, but we don’t know the answer yet.”
As a physical therapist, Davenport is focused on working with patients to find ways they can control and manage their symptoms.
One strategy involves having patients wear heart rate monitors throughout the day to track their exertion levels in real time.
“It’s like a crystal ball on your wrist. It gives you an idea if you’re putting yourself at risk,” Davenport explained.
Other approaches have been developed to improve blood flow to the heart and control heart rate abnormalities. He plans to conduct more formal research but has already seen results with long-COVID patients, including Park.
“If I hadn’t talked to him (Davenport), I don't know where I would be today,” Park said. “I think managing my heart rate and meditation helped a lot.”
Davenport has presented his findings nationally and internationally, including to the World Health Organization, in hopes of helping other patients.
The professors also participate in monthly Zoom meetings worldwide to share their knowledge with people who have long-COVID. A recent meeting held by a Norwegian chronic fatigue syndrome association had nearly 500 participants.
“It’s important to get this out to help people have better outcomes,” Davenport said.